JOHN SHUFELDT, MD, JD, MBA, FACEP The urgent care sector in particular, and healthcare in general, is undergoing a sea change—a phrase that has its origins in Shakespeare’s The Tempest: Full fathom five thy father lies Of his bones are coral made Those are pearls that were his eyes Nothing of him that doth fade But doth suffer a sea-change Into something rich and strange. Shakespeare was referring to the corpse of Ferdinand’s father being …
Read MoreHedging Your Bets: The Art of Market Segmentation
If you have more than one child or grew up with at least one sibling, you have probably experienced “segmentation.” That is, you have most likely used different tactics and strategies in dealing with each of your children or you were treated somewhat differently than your siblings. Segmentation within the urgent care occupational health market follows the same principle; a communication technique that is effective with one audience may not work as well with another. …
Read More
The Front Office: Window to Your Practice
Urgent message: Patients will return again and again—and tell their friends, too—if your center’s manager and employees are unfailingly courteous, com petent, and thorough. Alan A. Ayers, MBA, MAcc, Experity If you’re planning to own and operate an urgent care center, you’re probably not thinking about managing an administrative office. Instead, you envision yourself hurrying between exam rooms, suturing cuts, setting fractures, and dispensing orders. Digging your way out of paperwork, refereeing staff disputes, tracking …
Read More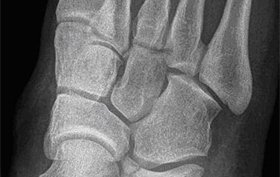
18-year-old male landed hard on heel
The patient is an 18-year-old male who jumped or fell from a \”short height\” but landed hard on his heel. He is able to ambulate, but cannot put any pressure on his heel. Examination and history reveal nothing remarkable. View the x-ray taken and consider what your diagnosis or next steps would be.
Read More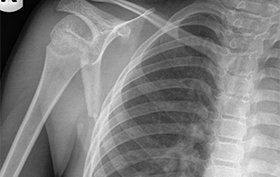
9-year-old boy injures shoulder in fall
The patient is a 9-year-old boy who received a blow to the shoulder from a height of approximately 6 ½ feet. He has limited elevation of the arm due to pain. Examination and history reveal no additional factors. View the x-ray taken and consider what your diagnosis or next steps would be.
Read MoreDeveloping Data: October, 2008
In Developing Data, JUCM will offer results not only from UCA’s annual benchmarking surveys, but also from research conducted elsewhere to present an expansive view of the healthcare marketplace in which urgent care seeks to strengthen its presence. In this issue: How did patients in a national study of visits to emergency departments in the United States rate their experience according to select key indicators of satisfaction? One can surmise from the data that participants …
Read MoreNebulizer Treatment Coding and Take-backs on 99051
DAVID STERN, MD (Practice Velocity) Q.Payors do not seem to want to pay on the code E0572 (aerosol compressor, adjustable pressure, light duty for intermittent use). What can we do to get payment? A.This code is not for simple use of the aerosol compressor, but is actually used to code for sale of the actual nebulizer machine. Thus, this code would rarely be appropriate for use in the urgent care setting. Q.How do we get …
Read MoreAbstracts In Urgent Care: October, 2008
A Short Video About What to Expect in the ED Increases Patient Satisfaction Key point: Showing the video to patients in the ED waiting room increased their satisfaction with the ED experience. Citation: Papa L, Seaberg DC, Rees E, et al. Does a waiting room video about what to expect during an emergency department visit improve patient satisfaction? CJEM. 2008;10:347-354. Assessment of patient satisfaction has become a component of physician and emergency department evaluation. Investigators …
Read More
October 2008
Occupational Health Sales and Marketing as a Team Sport
A thinly veiled secret in most urgent care clinics is the marginal role that sales and marketing plays in the mores of these organizations. Indeed, healthcare sales professionals tend to be like your Uncle Fred: it’s always nice to see him, but he’s not really woven into the inner fabric of your family. Why? To a large extent, urgent care owners have a hard time merging the healthcare side of their clinic(s) with the business …
Read More